An Overview of Melanoma: Identification, Causes, Treatment, Prevention.
On Jan 15, 2014
Look all over your skin and I bet you will find at least one or multiple moles. They may range in all different sorts of pigments, shapes and sizes. While some may be so miniscule, others may be harder to miss because of their large size and abnormal shape. What many people lack knowledge on is the fact that these seemingly harmless moles can just as easily turn into something malicious.
As reported by American Cancer Society and American Academy of Dermatology, skin cancer is the most common type of cancer, affecting one out of every five Americans. While melanoma is the least common type of skin cancer, as compared to basal cell and squamous cell carcinoma, it is the most deadly. Melanoma kills approximately 9,790 people in the U.S. annually according to the American Cancer Society. We urge our readers to be aware that no matter how big, small, or plain-appearing your moles may seem to you, your dermatologist is the best person to evaluate whether your mole has the risk of turning into a melanoma. This article will focus on the causes, treatment options and strategies for prevention for melanoma.
Identifying Melanoma
.jpg)
The ABCDE criteria for risk stratification of atypical moles.
Image Source: Flickr, user GIgi_QC
If you have no idea how to conduct a self-examination in order to find atypical moles, no need to fear. There is an article already published right here on Central Skin detailing the criteria used to recognize moles that may be atypical. But just to summarize, the categorization is known as the ‘ABCDE’ criteria, an abbreviation for asymmetry, border, color, diameter and evolution. If any of your moles seem irregular in any of the categories listed above, it is probably best to go see a dermatologist right away for a full-body skin exam and find out for certain whether your moles are benign or malignant.
The Causes
There are several risk factors that can lead to the development of melanoma. One major factor is overexposure to ultraviolet rays from the sun or tanning booths. In addition, your skin type can also determine whether you are more likely to be diagnosed with melanoma. If you are of fairer skin and have light-colored hair and eyes, you have an increased risk for the cancer. A major risk factors for melanoma is a family history of the disease in a first degree relative (your parents, your siblings). Also, older age and the male gender (usually above 50 years of age) are associated with an increased risk.
Melanoma may develop de novo (not from an existing mole) or it may form from a dysplastic or congenital nevus. Dysplastic nevi are moles which have atypical features such as irregular size, shape and color. Congenital nevi are moles that you are born with. While small congenital nevi have little risk, larger congenital nevi (20cm or greater) have a lifetime risk of turning into melanoma between 3.3-6.0%. Patients with atypical mole syndrome have the greatest risk of developing melanoma. Whether the moles are dysplastic or congenital, abnormal looking moles that meet any of the ‘ABCDE’ criteria should be examined by a dermatologist.
Treatment

Excessive exposure to UV rays is one of the major causes of melanoma. Image Source: Wikimedia
Various treatment options for melanoma exist today. If melanoma is caught early, before it has the chance invade deeply into the skin the subcutaneous tissue, a patient may be completely cured with a surgical excision.
Once melanoma has spread, or metastasized, to other areas of the body, it is usually fatal. However, there are some promising newer therapies available today which may target metastatic melanoma. One form of therapy is known as immunotherapy which activates one’s immune system in order to eliminate cancerous cells. One of the medicines used in immunotherapy to strengthen the immune system is a monoclonal antibody called Ipilimumab (Yervoy). The drug performs by blocking the immune-suppressing protein called CTLA-4, thus augmenting the body’s own immune system to fight off melanoma.
Another method is called targeted molecular therapy. This particular therapy uses drugs such as Vemurafenib (Zelboraf) to target the specific genetic mutations (the B-RAF gene) that allows melanoma cells to proliferate uncontrollably. Chemotherapy is yet another treatment option that is employed in the advanced stages of the cancer. Although chemotherapy is not curative, it may prolong a patient’s survival. One type of chemotherapy is isolated limb perfusion, typically performed during surgery. If melanoma is specific to just one area such as a patient’s arm or leg, the blood flow in that area can be temporarily cut off from the rest of the body. This allows surgeons to inject a high dose of a chemotherapy drug (usually melphalan) into the affected body part while minimize toxic side effects to the rest of the patient’s body.
Finally, radiation therapy is another option to consider for patients with melanoma. Unlike the above methods, radiation therapy is generally not used to treat the original source of melanoma. Instead the therapy is more commonly applied to areas of skin where moles were removed for surgery. This is a type of adjuvant treatment—or supplemental care after surgery—to assure cancerous cells will not return to the specified area. Radiation may also be used to treat relapsing melanoma and decrease the chances of it spreading elsewhere in the body.
Prevention
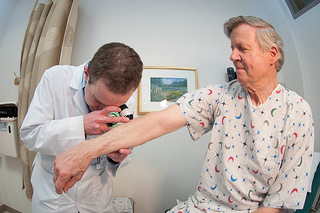
Preventative measures for melanoma are simple and involve using smart sun-protection strategies . To summarize, stay out of the sun whenever possible, avoid tanning booths, wear clothing or other accessories to shield your body and face from the sun. Also, examine your skin for any abnormal moles periodically. Self check-ups are not enough however, so we advise going see a skin specialist once every year for a full body skin examination.



Comments
Leave a Comment