Keratosis Pilaris - How to identify and treat this prickly problem.
On Jun 30, 2013
Keypoint Tweet@CentralSkin: Keratosis Pilaris: a prickly problem without an easy solution.
Chances are, either you or multiple people that you know have keratosis pilaris. It is an extremely common skin condition that many people do not know much about. Read on for 7 bits of knowledge about the diagnosis, causes, and treatments for this very common skin condition.
1. What is keratosis pilaris?
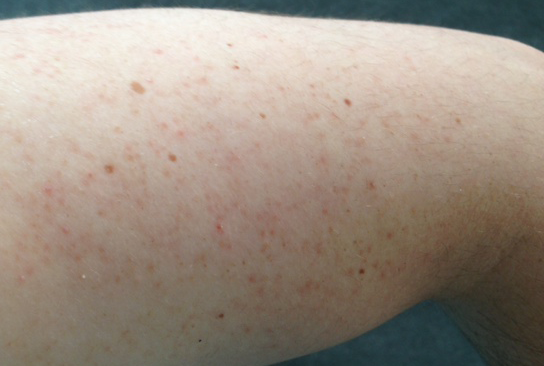
It is a condition where you develop rough patches of small horny bumps on the outer sides of your arms. Keratosis pilaris (KP) can also appear on your thighs, buttocks, and cheeks. The bumps can sometimes appear red and although they have a characteristic appearance, they do not itch or hurt. KP sometime gives the appearance of chicken skin.
2. What skin conditions mimic keratosis pilaris?
Atopic dermatitis, also known as eczema, is associated with KP. Atopic dermatitis can also give your skin a rough, dry appearance. However, unlike KP, atopic dermatitis frequently affects the insides of your arm and the back of your knees. Also, atopic dermatitis usually presents with rough, “thickened” dry appearing skin and rarely presents with prickly distinct bumps as KP. Folliculitis is a bacterial infection of your hair follicles that can sometimes look like KP. However, unlike KP, folliculitis usually has some small pustules (small bumps filled with white pus) and is usually not symmetrical in distribution such as KP. Milia are tiny keratin filled cysts that can sometimes look like KP. However, milia are usually distributed on facial skin and are much more common in infants than older children and adults like KP. There can be other skin conditions that may mimic KP and so the best option for you is to make an appointment with a dermatologist to properly diagnose your skin condition.
3. Who can I blame for having keratosis pilaris?
You can blame your parents since KP is passed down to you genetically. It is inherited in an autosomal dominant fashion, meaning that if one of your parents has it, you have a 50% chance of getting KP. KP is also very common, with some estimates suggesting that it effects up to half of the adult population and 50-80% of the adolescent population.
4. What causes keratosis pilaris?
KP results from an excess production of keratin, the main protein found in your skin, nails, and hair. Excess keratin builds up and forms hard plugs inside your hair follicles. This results in the characteristic appearance of tiny horny keratin filled plugs which feel like rough patches of skin.
5. Is it the same as goosebumps?
While KP may have the same prickly appearance as goosebumps, the two conditions are not related. Goosebumps occurs because of the contraction of tiny muscles associated with your hair follicules called arrector pili. Arrector pili muscles get activated by your sympathetic nervous system in situations of extreme intense emotion or very cold temperature.
6. Are there any long term health risks I should worry about if I have keratosis pilaris?
No, other than the cosmetic effects, KP does not have any long term consequences for your health. That being said, since there are other skin conditions which may mimic KP, it is best to get a true diagnosis by seeing your dermatologist.
7. How do I treat this prickly problem?
KP can resolve without treatment and people who develop KP in their childhood frequently see it diminish or disappear by the time they turn 30. However, this is not the case for everyone. For those looking for a cure, we have bad news for you. Unfortunately there are no “cures” to KP and most treatments don’t completely eliminate the condition. That being said, there are multiple skin care routines and over-the-counter and prescription treatments which may keep KP at bay. Self help measures include keeping your skin very moisturized and applying moisturizers on your skin while it is still moist immediately after you get out of the shower. In addition, avoid scrubbing of the rough patches of skin, as this may cause irritation and make your skin redder. Also, gently dry off with your towel instead of vigorous drying to make sure that there is some moisture left on the dry areas. You can also apply over-the-counter creams such as AmLactin or Lac-Hydrin twice a day to the affected areas. These creams gently act to exfoliate your skin and remove the excess keratin. For stronger exfoliation, your dermatologist may prescribe you a topical 40% urea cream. In addition, your dermatologist may prescribe you a topical vitamin A derivative called a retinoid (such as Retin-A). This medication promotes a more rapid skin turnover and prevents follicle plugs from forming. Certain types of KP may also respond to laser therapy. Since most treatments have both benefits and side effects, see your dermatologist to discuss the most appropriate treatment options for your condition.


Comments
Leave a Comment